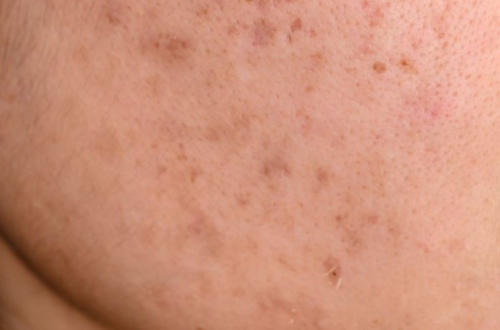
If you’ve been layering serums, switching cleansers, and praying to the skincare gods, yet those tiny, itchy bumps just won’t disappear, I feel you. There’s a special kind of frustration that comes with doing everything right and still waking up to new breakouts. But here’s the twist: what if those spots aren’t acne at all?
A lot of people go years thinking they’re battling hormonal or bacterial acne when they’re actually dealing with fungal acne (scientifically known as Malassezia folliculitis). It’s sneaky, stubborn, and ridiculously misunderstood. So, let’s break it down, here are 10 subtle signs your breakouts might actually be fungal acne, plus what you can do about it.
1. Your “acne” itches and not in a mild way
Regular acne usually hurts. Fungal acne? Itches like a rash that’s holding a grudge. If you’ve ever felt the urge to scratch your cheeks, back, or forehead because of those little bumps, that’s a red flag.
Why it happens: The yeast (Malassezia) responsible for fungal acne feeds on oil and humidity, causing inflammation and itching. It’s like your pores are hosting an unwanted yeast party.
Also, please take a moment to follow us on pinterest, your support helps us to put out more content like this. Thank you!
2. The bumps look small, uniform, and kind of… identical
You know how typical acne has a mix of blackheads, whiteheads, and those painful cysts? Fungal acne doesn’t play that game. The bumps all look the same, small, clustered, and usually filled with pus.
Quick tip: They often appear in straight lines or tight clusters instead of random patches. Think tiny, even-textured bumps instead of sporadic spots.
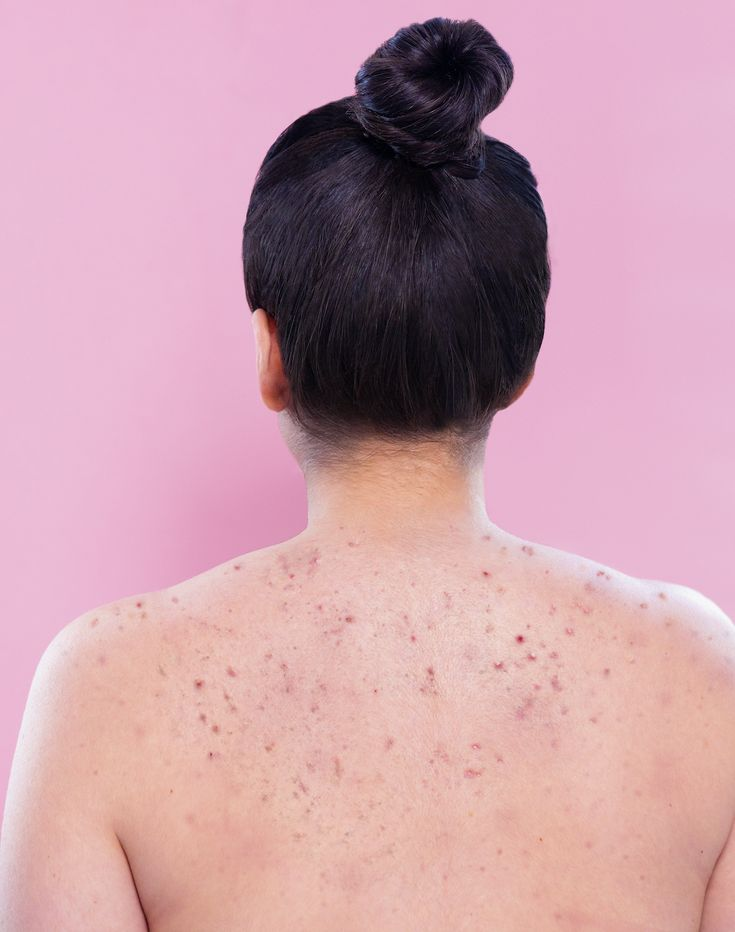
3. It shows up on your chest, back, shoulders, or hairline
While hormonal acne loves your chin and jawline, fungal acne has a thing for your upper body. It thrives in warm, sweaty areas, like your chest, back, shoulders, or along your hairline.
If your face is mostly clear but your upper body has small itchy bumps that seem to get worse after sweating, chances are high that it’s fungal.
4. Sweat makes it worse
You know that post-workout glow everyone talks about? Yeah, fungal acne didn’t get the memo. If your skin gets worse after you sweat or wear tight gym clothes, that’s a sign.
Why: The yeast causing fungal acne loves moisture and warmth. So when you trap sweat under clothing or skip showering right after the gym, it’s basically a yeast buffet.
What helps: Use an antifungal body wash like Nizoral Anti-Dandruff Shampoo (with Ketoconazole) on the affected area 2–3 times a week. Leave it on for a few minutes before rinsing. Works wonders.
5. Antibiotics make it worse instead of better
If you’ve used antibiotic creams or pills and your “acne” got worse, that’s another clue. Antibiotics kill bacteria but fungal acne isn’t bacterial, so what happens? You wipe out the good bacteria that normally keep yeast in check.
The result? The yeast grows even faster. Classic plot twist.
6. Your skin feels bumpy but not inflamed
Unlike cystic acne, fungal acne doesn’t always cause deep inflammation. You might run your hand across your forehead or cheeks and feel tiny sandpaper-like bumps, yet your skin doesn’t look particularly red or angry.
It’s that confusing in-between texture that just won’t smooth out, no matter how many exfoliants you use.
7. You’ve tried everything and nothing works
If you’ve used benzoyl peroxide, salicylic acid and retinol, but nothing works, it’s time to suspect fungal acne.
Those ingredients target bacteria and oil, not yeast. In fact, overusing them can irritate your barrier and make the problem worse.
FYI: Fungal acne doesn’t respond to traditional acne treatments. You need antifungal ingredients like sulfur, zinc pyrithione, or ketoconazole to actually kill the yeast.
8. It flares up during humid weather or after sweating
If your breakouts seem to follow the weather forecast, clear in dry seasons and worse during hot, humid days that’s a sign.
The yeast causing fungal acne thrives in damp, warm conditions. So when humidity hits, your pores basically turn into a spa for them.
Pro tip: Try using a lightweight, oil-free moisturizer. Products like La Roche-Posay Toleriane Double Repair Matte Moisturizer or CeraVe PM Lotion help balance hydration without feeding the yeast.
9. Your skincare routine is heavy on oils or occlusive products
Love facial oils? Same. But if you’re prone to fungal acne, some oils might be your enemy. Yeast feeds on certain fatty acids, especially in coconut oil, olive oil, and cocoa butter.
If you’ve recently started using richer creams or sleeping masks and suddenly your breakouts worsened, check those ingredient lists.
What to do instead: Switch to non-comedogenic and fungal-acne-safe options like squalane, hemp seed oil, or neem oil they’re light and don’t fuel yeast growth.
10. It responds to antifungal products fast
The final giveaway: when you switch to antifungal treatments and your skin suddenly clears up.
If using Nizoral shampoo, Head & Shoulders (zinc pyrithione), or even sulfur-based masks makes your breakouts vanish within a week or two, congratulations, you’ve cracked the code.
That’s the ultimate confirmation that you were dealing with fungal acne all along.
What Actually Causes Fungal Acne?
Fungal acne isn’t caused by dirt or bad hygiene (let’s kill that myth right now). Everyone has Malassezia yeast living on their skin it’s part of your natural microbiome. The issue starts when it overgrows, usually due to:
- Sweat buildup and tight clothing
- Overuse of antibiotics or acne treatments
- Heavy, oil-based products that feed the yeast
- Hot, humid environments
- Weakened skin barrier
Basically, when your skin’s balance tips out of control, yeast takes advantage and throws a breakout party.
How to Treat Fungal Acne (and Keep It Gone)
1. Cleanse with antifungal ingredients:
Use shampoos like Nizoral or Head & Shoulders as body washes 2–3 times weekly. Let them sit on your skin for about 3–5 minutes before rinsing.
2. Try sulfur-based products:
Sulfur naturally kills yeast and calms inflammation. Try the De La Cruz Sulfur Ointment or Kate Somerville EradiKate Mask for mild cases.
3. Simplify your skincare routine:
Ditch the twelve-step routine for now. Focus on gentle cleansing, hydration, and protection. Overdoing actives can weaken your barrier and invite more yeast.
4. Avoid high-fatty-acid oils:
Skip coconut oil, shea butter, and olive oil if you’re prone to fungal acne. Opt for squalane, mineral oil, or lightweight gels instead.
5. Shower after sweating:
This one’s easy but crucial. Showering right after a workout (and changing out of sweaty clothes) keeps yeast from multiplying.
6. Add an antifungal cream if needed:
If things get stubborn, OTC creams with clotrimazole or ketoconazole can help. Apply to the affected area daily for 1–2 weeks.
When to See a Dermatologist
If you’ve tried antifungal products for a couple of weeks and your skin isn’t improving, it’s time to get professional help. A dermatologist can confirm the diagnosis and prescribe stronger oral antifungals like fluconazole if needed.
Remember, it’s better to treat the actual cause than to keep guessing.
Final Thoughts
Fungal acne can make you feel like your skin is betraying you, especially when you’ve tried everything and nothing seems to work. But once you understand the signs, it’s honestly liberating. You stop wasting money on the wrong treatments and finally start healing your skin.
So, if you’re staring at those stubborn bumps right now thinking, wait a minute…, trust your gut. Sometimes, the solution isn’t more exfoliating or new serums, it’s just knowing your enemy. 🙂